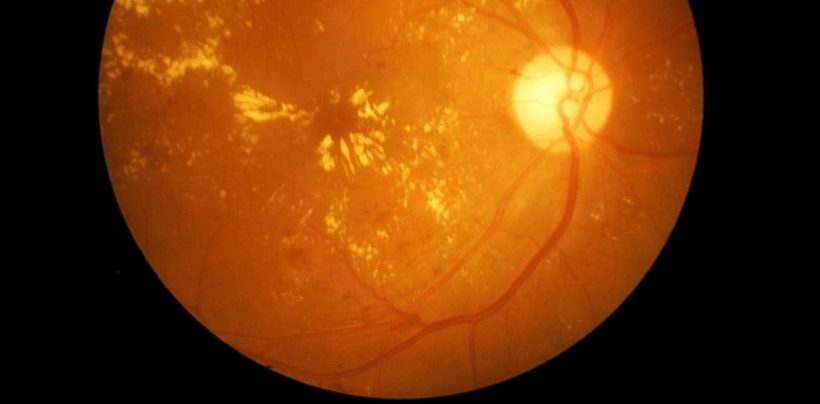
The single most expensive drug for the Australian government today, costing more than A$400 million per year, is one called aflibercept. It stops the growth and “leakiness” of blood vessels, and is given to treat a range of different eye diseases. These diseases have one thing in common: they all affect a piece of tissue inside the eye called the macula.
The macula is a structure that distinguishes us humans, as well as some other primates including apes and monkeys. It is a part of the retina that lets us recognize people’s faces, navigate a car and read the newspaper. Our eye is built to focus images onto the macula to achieve this level of vision.
Like the rest of the retina, the macula consists of cells that detect light—photoreceptors—plus nerve cells and other supporting cells, but they are arranged differently to ensure images are seen in high resolution. The macula also contains the highest body concentration of yellow carotenoid pigments—protective antioxidants which filter out blue light to hone vision.
Scientists are working to understand why so many diseases and conditions, including diabetes, inflammation and parasitic infection, affect the macula. This is likely due to a host of factors: from the special anatomy of cells, to blood supply, the need for carotenoid pigments and a high metabolic rate.
The many causes of macular disease
When a person’s macula becomes diseased, they often experience changes in vision. However, because the macula is just one part of the retina, even severe macular disease generally does not cause complete loss of sight.
Dame Judi Dench has talked about her macular disease—macular degeneration—including how friends help her learn lines by repeating them over and over to her, and how fellow performers help her know where to face when she is acting. Having this condition might mean she no longer drives a car, but she continues to live a full life.
Macular degeneration affects about one in seven people over 50 years of age, and can occur as an overgrowth of blood vessels or as a loss of tissue.
Diabetes causes an accumulation of fluid in the macula, called macular oedema; around one in 15 people with diabetes develop this condition. Other causes of macular oedema include a blocked blood vessel or inflammation inside the eye. It can also be a complication after cataract surgery.
There are many more macular diseases.
- Toxoplasmosis—a parasite infection—often affects the macula.
- Macular disease is a side effect of some drugs, such as hydroxychloroquine used to treat inflammatory diseases like lupus, and the new immunotherapy drugs for cancers including melanoma.
- Central serous chorioretinopathy is a macular disease that affects younger adults and is associated with high levels of the stress hormone cortisol. Rare inherited conditions can affect the macula even earlier in life.
Treatments and prevention: Five ways
Treatments depend on the type of macular disease. Most drugs are given by injection with a fine needle into the back part of the eye, called the vitreous. This quick procedure may be done in the doctor’s office.
But understanding what the causes of disease have in common points to lifestyle changes that can protect the macula or slow the damage of diseases.
1. Diet
Researchers at the United States National Eye Institute have shown the benefits of a Mediterranean diet, heavy in legumes and other vegetables, fruits, nuts and whole grains, and favoring fish over red meat, for protection against macular degeneration. A supplement combining vitamin C and E, lutein and zeaxanthin, zinc and copper is also recommended to limit progression of certain types of degeneration.
2. Avoiding smoking
Not taking up smoking or quitting if you are already a smoker safeguards your macula. Smoking has been linked to a number of macular diseases, including macular oedema and central serous chorioretinopathy, as well as macular degeneration.
3. Sun smarts
Wearing a sunhat and sunglasses from childhood may have benefits beyond skin safety. Some studies suggest sunlight exposure is a risk factor for macular degeneration. Physical activity can also protect against this condition, although there is debate about whether vigorous exercise is protective or potentially dangerous.
4. Shut eye
Quality sleep protects the macula. Sleep apnea is associated with several macular diseases, including macular degeneration, macular oedema and central serous chorioretinopathy. Moreover, people with these diseases and untreated sleep apnea may need more frequent drug injections for their condition.
5. Busting stress if possible
Limiting stress in life is difficult, but stress is a well-established risk factor for central serous chorioretinopathy. One group of U.S. researchers reported an unusually high number of people with the disease at their local health network early in the COVID pandemic, which was a highly stressful time.
Controlling other aspects of diseases that affect the macula can be important too. For example, the macula benefits from: keeping blood pressure well-controlled, stabilizing blood sugars in people with diabetes, and reducing inflammation in people with uveitis.
Check it and see
You can monitor your own macula using a simple test called the Amsler grid, available for free online.
Testing with an Amsler grid picks up changes in the vision caused by macular diseases.
Self-testing doesn’t take the place of regular checks with your eye health practitioner. They can examine your macula directly, usually after dilating the pupils, and may employ a powerful technology—optical coherence tomography—to scan through it.
Provided by
The Conversation
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Source: Read Full Article